 
Therefore, a modified transfibular approach, called ‘partial fibular head osteotomy’ ( Figure 1), was developed to manage posterolateral tibial plateau fractures. Some studies have reported that the transfibular approach has no adverse effects ( 3, 11), while others reported some disadvantages, such as common peroneal nerve injury, fibular nonunion, and destabilization of the proximal tibiofibular joint ( 10). The transfibular approach (fibular head osteotomy or fibular neck osteotomy) can intuitively expose posterolateral articular injuries. However, this approach usually causes more soft tissue damage, such as knee posterolateral ligament complex injury, common peroneal nerve injury, and inferolateral geniculate artery injury ( 10). The posterolateral approach can visualize the posterolateral articular surface, manage posterolateral fracture fragments, and provide posterior implants for effective fixation ( 9). However, this approach has limited exposure for fractures involving the posterolateral articular surface and does not permit the insertion of posterior fixation ( 8). The standard anterolateral approach can be used to visualize the articular surface and manage lateral fracture fragments of the lateral tibial plateau. 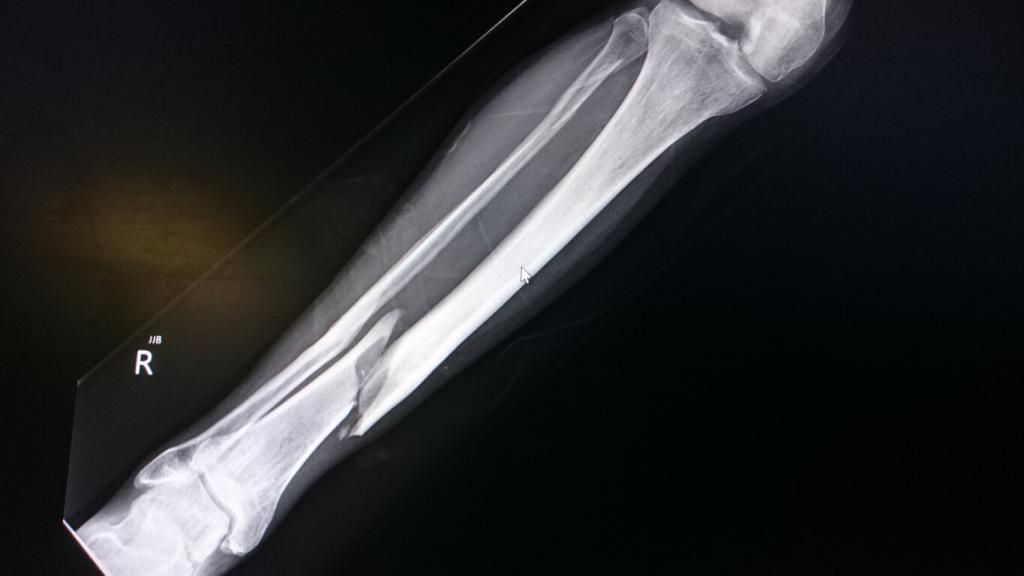
A variety of approaches have been used for open reduction and internal fixation of posterolateral tibial plateau fractures ( 3, 5– 7). For intra-articular fractures, anatomic reconstruction of the articular surface and fixation for displaced posterolateral fractures of the tibial plateau are important for knee joint range of motion and stability ( 3, 4). Isolated posterolateral tibial plateau fractures are rare and often part of complex tibial platform fractures ( 2). Posterolateral tibial plateau fractures remain a great challenge for orthopedic surgeons ( 1). One patient had a superficial infection and was treated with surgical dressing.Ĭonclusion: The partial fibular head osteotomy approach is a feasible alternative for treating posterolateral tibial plateau fractures. None of the patients exhibited symptoms of common peroneal nerve injury, knee instability, or upper tibiofibular joint injury. The mean HSS at the final follow-up was 93.5 ± 5.4 (range, 79–100). The mean time from injury to surgery was 3.1 ± 1.8 (range, 1–10) days. Fracture united in all patients and the average clinical healing time for fractures was 11.2 ± 1.9 (range, 8–16) weeks. Results: The mean follow-up period was 21.5 (range, 12–36) months. Knee joint function was evaluated using the Hospital for Special Surgery Mayo Score (HSS). The mode of injury, time from injury to surgery, time for fracture union, range of motion of the knee, and complications were recorded. Computed tomography was performed for fracture typing and evaluation. Methods: A retrospective analysis was performed on 25 patients with posterolateral tibial plateau fractures who were treated using a partial fibular head osteotomy approach. Objective: This study aimed to evaluate the short-term effects of partial fibular head osteotomy for treating posterolateral tibial plateau fractures. 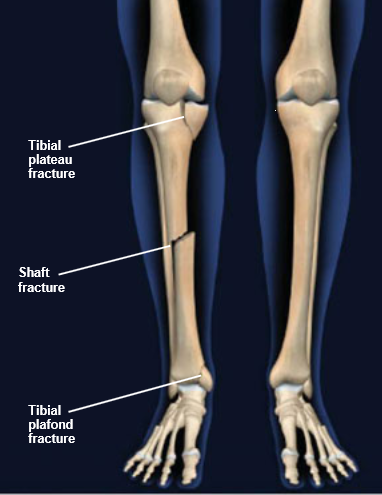
3Orthopaedics Institute of Chinese PLA, 80th Hospital, Weifang, China.2Bioinspired Engineering and Biomechanics Center (BEBC), The Key Laboratory of Biomedical Information Engineering of Ministry of Education, School of Life Science and Technology, Xi’an Jiaotong University, Xi’an, China.1Department of Orthopaedic Surgery, Honghui Hospital, Xi’an Jiaotong University, Xi'an, Shaanxi, China.Yao Lu 1,2† Gen Wang 3† Cheng Ren 1† Yibo Xu 1 Qiang Huang 1 Shan Fan 1 Ming Li 1 Kun Zhang 1 Zhong Li 1 Qian Wang 1* Teng Ma 1*
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
